How diversifying and supporting clinical teams can help solve healthcare’s DEI problem
The life sciences sector is constantly striving to launch safe, effective and profitable solutions. However, 30% of all recently launched pharmaceuticals have failed to meet market expectations. A study by Deloitte found that a lack of understanding of customers (patients and prescribers alike) and their needs is one of the biggest reasons for this failure.
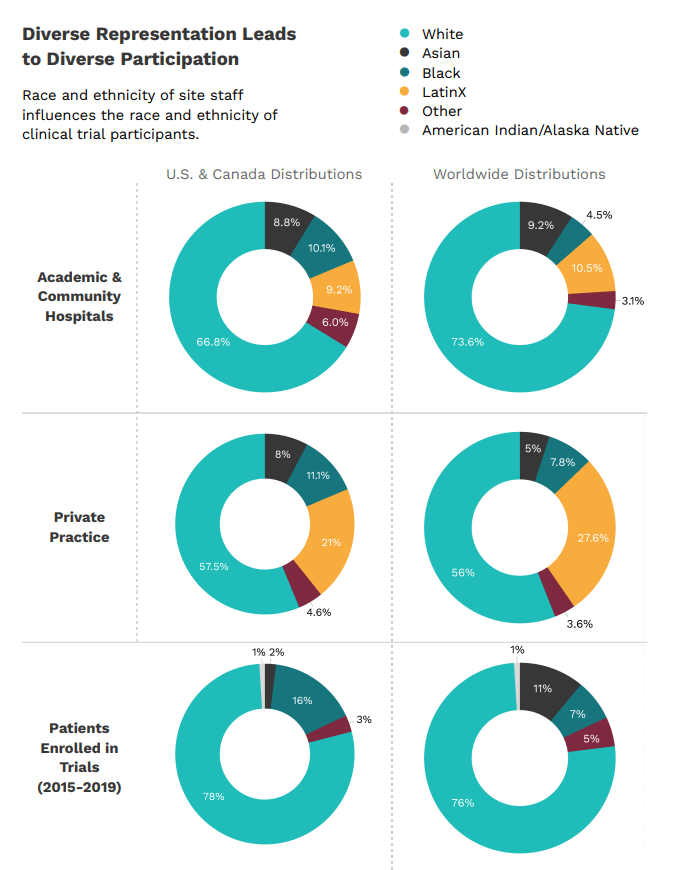
We know diverse clinical trial participation matters. Increasing site diversity is fundamental to public health and is not limited to patient participants. Clinical trial sites face challenges in diversifying personnel, including principal investigators (PIs), sub-PIs, trial coordinators, etc.
Removing obstacles to DEI
At Inlightened, we believe that healthcare innovation — including the development of better solutions and improved ways to combat diseases — starts at the top, with diverse expert insights. By engaging these professionals throughout the innovation lifecycle, organizations can ensure that their solutions are safe and effective for a broader range of patients. Including and prioritizing diverse perspectives can help identify potential issues and build trust with underrepresented communities, leading to better patient outcomes, improving the launch’s overall success, and supporting long-term performance.
Here’s what our Inlightened experts think about building trust and advancing health equity to ensure a brighter future for all, not just the over-represented few.
Upstream impacts of care team creation and community participation
“As we seek to address the inequities in healthcare, the upstream impacts of how our care teams are built and how medical interventions are created and preferably targeted needs to be prioritized. With worsening chronic disease, cancer screening and treatment, maternal mortality, and other significant areas, impacted marginalized communities require more than improved access to care; they need to be involved in all facets that will lead to solutions. We need increased participation in the healthcare workforce and leadership, and a hand in developing the solutions that will help us — through the ownership and participation in clinical trials.
Whether pharmaceutical or digital interventions, marginalized communities have lost trust in the larger academic and commercial efforts that historically deprioritize the needs of the individuals involved in their development. Health equity must begin upstream by expanding community participation in all facets of clinical trials through culturally humble outreach and transparency.”

Kameron Leigh Matthews MD, JD, FAAFP, is a board-certified family physician and Chief Health Officer of Cityblock Health, a transformative, value-based healthcare provider integrating medical, behavioral, and social services for Medicaid and dually eligible and low-income Medicare beneficiaries. Dr. Matthews has focused her career on underserved and vulnerable communities, having held multiple leadership roles in correctional medicine, federally qualified health centers, and managed care. As a passion outside of work, Dr. Matthews co-founded and co-directs Tour for Diversity in Medicine, an initiative seeking to bring premedical enrichment activities to underrepresented minority high school and undergraduate students across the country.
Workplace diversity, from residency to patient outcomes
“Diversity in the workplace brings many benefits for healthcare employers, their staff, and their patients. Bringing together healthcare staff with diverse experiences, cultures, and backgrounds improves organizations’ ability to ideate, problem-solve, and empathize with patients.
Our patient population is not homogenous. Our patients come from many different socioeconomic backgrounds and racial and ethnic backgrounds. Many also have language barriers. Therefore, it is essential to have a diverse healthcare force that represents the patients we treat. Studies have shown that physician-patient racial or language concordance correlates to improved patient satisfaction and adherence.
Creating a diverse workplace is important for medical students applying for residency. A study of 2008–2017 residency match data showed that an impressive 33.8% of applicants cited diversity as a factor in program ranking, an increase of more than 10% in the last decade.”

Jennifer Harris, MD, is an Ivy League trained and board-certified neurologist at Cedars-Sinai Medical Center, where she also serves on faculty for the Neurology Residency Program. Dr. Harris specializes in vascular neurology, treating patients affected by ischemic stroke, hemorrhagic stroke, TIA, carotid disease, and intracranial atherosclerotic disease. Passionate about health equity and eradicating disparities in care, she is uniquely attuned to urban medicine and belongs to Cedars-Sinai’s Diversity and Inclusion Committee.
Going beyond cultural competency to include the individual
“Patients present not only with varied healthcare needs but also expectations and beliefs, some of which are socio-culturally determined. Clinicians, in turn, possess expectations and beliefs that are shaped both by their professional training and experience, as well as by their social environment and broader societal norms that they inherit during their interactions with society. Diverse clinical teams bring a wider variety of experiences and perspectives, which help to understand patients better and as a result, inform clinical decisions better. They also help to avoid stereotyping patients based on their ethnic or racial background, as members of a more diverse team can pinpoint situations when a patient is not getting optimal treatment.
Patients’ trust is higher when interacting with clinicians from similar ethnic and racial backgrounds; they are more likely to raise concerns if they don’t feel heard and understood. Overall, cultural competency is not enough. Patients are more satisfied with the care they receive due to engaging with clinicians who devote themselves to treating the individual.”

Kasia Hein-Peters, MD, is an internationally-educated physician executive and innovation consultant. She boasts more than three decades of life sciences expertise in developed and emerging markets, with specific experience leading brand building initiatives, managing product lifecycles, developing integrated stakeholder engagement campaigns, and developing enterprise strategies. With a global understanding of complex healthcare ecosystems, Dr. Hein-Peters has played an integral leadership role across pharmaceutical, medical device, and digital health organizations. This includes serving as an advisor to Amah Health, providing science-backed communication strategies and tools to help healthcare teams to address patient beliefs and preferences.
Michelle Higginson, MBA, is an accomplished operator and marketing professional, with more than a decade of diverse experience that spans tech and healthcare sectors. She spent her early career contributing to exponential growth in fast-paced startup environments, and was instrumental in launching the content marketing and customer advisory board practices for LogMeIn, one of the world’s top 10 SaaS companies. Michelle then led marketing and communications for the Heart Center and Pediatric Transplant Center at Boston Children’s Hospital, where she directed multiple award-winning campaigns, pilots and initiatives, from concept through execution. She returned to the startup space as Director of Marketing at HBS-founded Avant-garde Health before co-founding Inlightened. Michelle serves on the board of Easterseals of Massachusetts, committed to supporting disabled individuals and veterans with opportunities to live, learn, work, and play.




